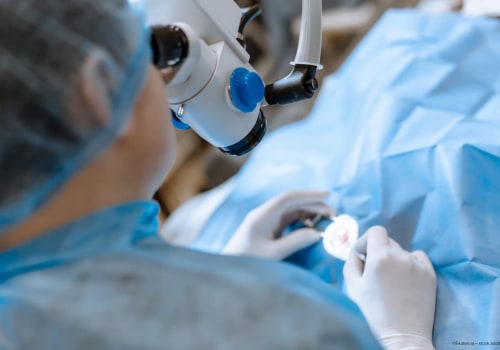
When considering cataract surgery, it is essential to be aware of the potential complications that may arise. These include retinal detachment, posterior capsule opacification, and infection. To be fully prepared for what is to come, it is important to understand the risks associated with the procedure.
Retinal Detachment
Retinal detachment (RD) is a common complication after cataract surgery, occurring at a rate 10 times higher than in the general population. It is caused by subretinal fluid accumulation between the neurosensory retina and the underlying retinal pigment epithelium, which can lead to dramatic deviations from expected visual outcomes. Research has identified three primary
risk factors for RD: male gender, age, and lattice degeneration. In addition, changes in vitreous anatomy and volume can contribute to the initial heightened risk. One study found that the cumulative probability ratio of RD remained four times higher than in the general population after 20 years. Another study evaluated risk factors for retinal detachment after phacoemulsification. The authors found that a longer axial length was associated with a higher risk of RD, but that the risk decreased after six months. Younger patients were also found to be at a greater risk of RD, although the reasons for this are still unclear. A Taiwanese study of 9,398 cataract surgeries revealed an overall incidence of RD of 0.62%.
Inflammation
Early postoperative inflammation following cataract surgery can have an impact on visual outcomes, although its effects are still not fully understood. Cystoid macular edema (CME) is rare after surgery but should still be monitored. It is important to determine if there is a correlation between the level of anterior chamber (AC) inflammation and the risk of developing CME in order to decide whether to start a treatment regime that effectively controls the inflammatory response after surgery. Anterior segment optical coherence tomography (AS-OCT) is an objective measurement of AC inflammation and can be used in clinical trials to assess whether there is a significant correlation between inflammation intensity and CME likelihood. A combination of topical NSAIDs and steroids was tested for reducing early postoperative inflammation in a small prospective randomized controlled trial; monotherapy with a topical NSAID was found to be most effective. A sub-Tenon depot of steroids was also studied in dropless cataract surgery but did not provide any additional benefits. The SUN scoring system is one of the most widely used methods for assessing inflammation after cataract surgery; however, it may not be applicable in patients with a predisposing etiology such as uveitis.