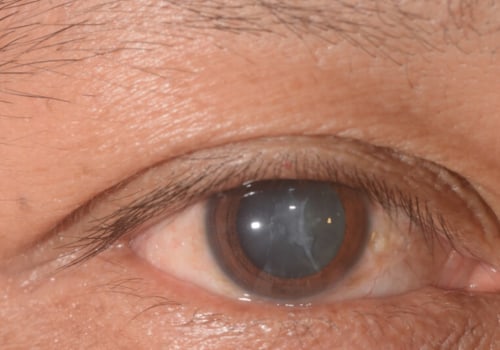
A long-term consequence of cataract surgery is posterior capsular opacification (PCO). PCO is the most common complication of cataract surgery. The most common complication of cataract surgery is inflammation of the cornea or the outer window of the eye. It can also cause more serious problems, such as bleeding and swelling.
You may need surgery to return it to its position or to place it in a new position. It's rare, but during surgery, the blood vessels that supply the retina may start bleeding for no reason. A little bit of blood isn't a problem, but larger amounts can cause vision loss. Swelling, bleeding, or excess lens fragments can cause increased pressure on the eye, which can cause glaucoma.
If possible, it may be beneficial to evaluate and treat other eye problems before making a decision to undergo cataract surgery. If you have cataracts in both eyes, your doctor usually schedules the second surgery after the first eye has healed. Several studies compared the rates of adverse effects as surgeons went from intracapsular cataract removal surgery (ICCE) to extracapsular cataract extraction (ECCE), and of the two procedures, ECCE has generally had the best safety profile. Cataract surgery remains a very safe surgical procedure, and few patients experience serious adverse effects that endanger their sight.
Occasionally, surgeons perform cataract surgery the same day with another intraocular procedure, such as penetrating keratoplasty, trabeculectomy, or pars plana vitrectomy. They were reported to be almost twenty times more likely to suffer from RD after cataract surgery when the back capsule ruptured. Ocular hypertension, an increase in pressure in the eye, is one of the most common risks of cataract surgery. During phacoemulsification, the most common type of cataract surgery, the tip of the ultrasound probe, which vibrates quickly, emulsifies and helps break up the cataract, which is then suctioned by the surgeon (top).
He conducted a case-control study with 249 patients with pseudophacic RD and 845 matching controls who underwent cataract surgery and discovered that a different surgical technique (ECCE) compared to cataract surgery consists of removing the lens from the eye and, in most cases, replacing it with an artificial lens. In an analysis, which used claim data from patients undergoing cataract surgery at Veterans Administration Medical Centers (VAMC) across the country, Greenberg et al. Several researchers have studied the rates of intraoperative and postoperative complications among cataract surgeries performed by resident surgeons. The most common intraoperative complication associated with cataract surgery is the alteration of the posterior capsule, which can cause loss of the vitreous, the need for a vitrectomy, the placement of the intraocular lens in the ciliary sulcus or the anterior chamber and, sometimes, the need for additional surgical interventions.
Numerous studies have evaluated the risk of RD after cataract surgery and the risk factors associated with pseudophachic and aphachic RD. In a study conducted at the Aravind Eye Hospital, one-year rates of serious postoperative complications were more frequent with ICCE surgery (14.5%) than with ECCE surgery (7.7%).